18/02/2026
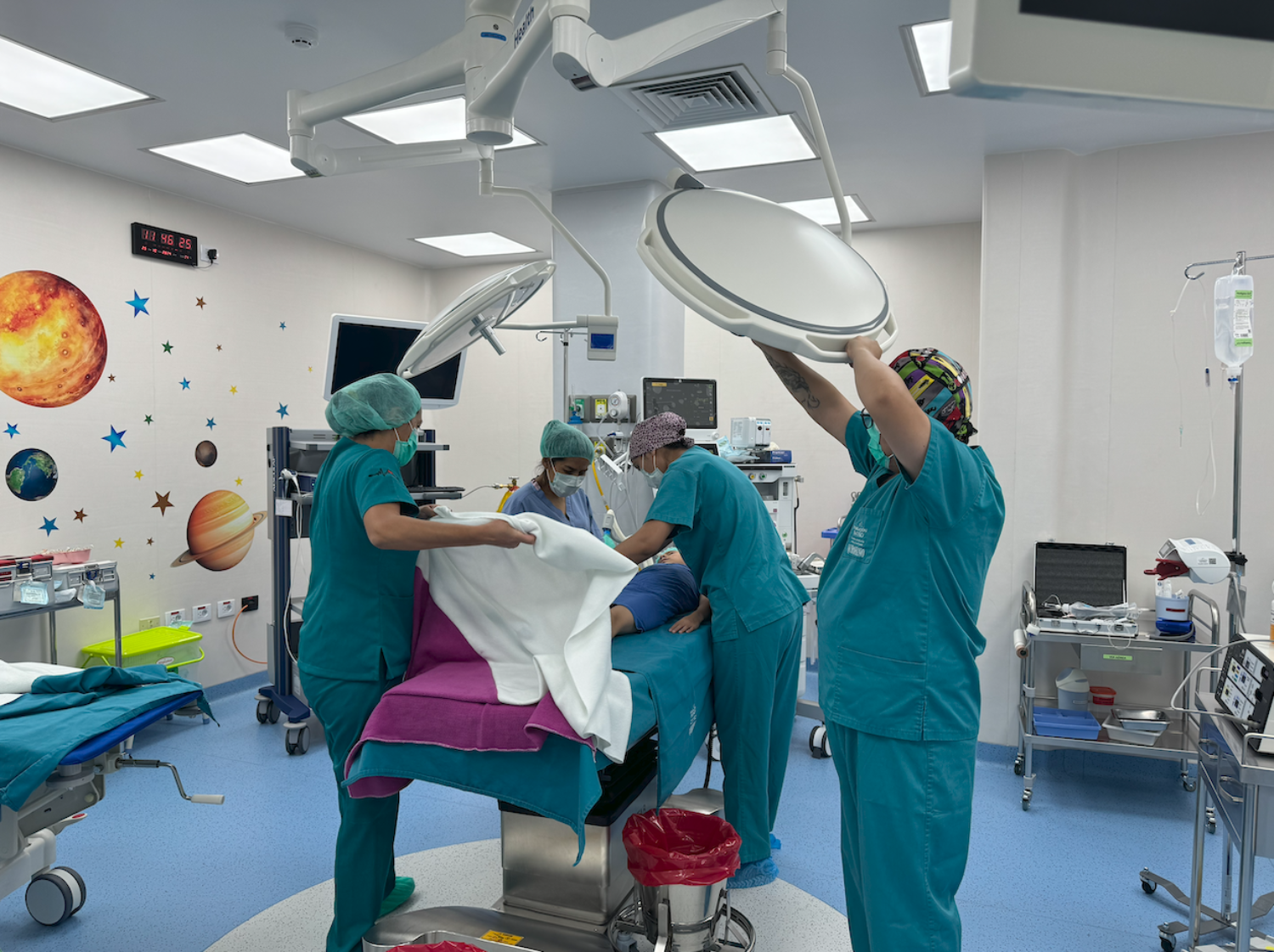
Reconstructive surgery of the sequelae of burns at the CPAP.
A burn is never a mere accident. In a child, it marks the body, yet it marks above all a trajectory. It interrupts a gesture, restrains a movement, exposes a skin too soon, for too long. It inscribes itself within duration. In childhood, and sometimes for life. In Bolivia, childhood burns are for the most part domestic. Water or oil heated upon the ground, a kitchen that shares its space with the sleeping room, a moment of inattention in a daily existence already under strain. Nothing spectacular. Nothing deliberate. Yet enduring consequences.
“These are seldom spectacular accidents. They are kitchens too close at hand, ordinary gestures, and a single moment that suffices.”
At the Albina R. de Patiño Centre of Paediatrics (CPAP), in Cochabamba, these histories arrive each week. And with them, a central question: what is to be done when the emergency has passed, yet the scar, for its part, remains?
This article is founded upon an in-depth exchange with a plastic and reconstructive surgeon of the CPAP, engaged for several years in the management of the sequelae of burns in children.
The Burn, a Silent Fracture of Childhood
A severe burn is a manifold assault—chemical, electrical, thermal. Yet in a child it is above all an assault upon development. According to its depth and its location, it may hinder growth, immobilise a joint, impede a natural movement. The most frequent sequelae concern the most visible and most functional regions: the hands, the neck, the face. A contraction about the mouth may obstruct alimentation. A cervical scar may restrict the mobility of the head. A peri-orbital burn may alter the gaze, the expression, the relation to another.
To these physical injuries is added a reality less visible, yet no less decisive: the psychological impact. At school, children are seldom indulgent. Scars draw the eye, and at times derision. What is not repaired upon the body often comes in the end to weigh upon self-esteem. To repair a burn, therefore, is to repair far more than skin.“A scar ill tended restrains not merely a movement; it restrains a childhood.”
Reconstructive, because both functional and human
At the CPAP, the surgery of burn sequelae pertains to reconstructive surgery—a discipline that does not choose between function and appearance, for the two are inseparable. To restore mobility without heed to aesthetics is to create a new limitation. To correct a scar without rendering a gesture possible is to disregard the body’s use. Each surgical decision engages both dimensions. This entails a high degree of technical mastery, but also a long-term vision. The incisions, grafts, and plasties are conceived to accompany the child’s growth, to limit recurrences, and to preserve the body’s natural lines. This requirement, however, encounters a reality well known to developing health systems: access to equipment. Certain instruments, standard elsewhere, here mark the difference between an acceptable solution and an optimal one. A simple dermatome—an instrument that permits the even harvesting of skin for grafts—can transform the quality of a reconstruction. Its absence compels recourse to more artisanal, more time-consuming, and at times less precise solutions. In this context, each material advance becomes a structural lever.
A Medicine of Teamwork, Never Solitary
“Surgery is but a cog in the mechanism. Without the paediatric team around it, nothing functions.”
Paediatric reconstructive surgery is never reduced to an operative gesture alone. It rests upon a precise mechanism, wherein each role bears its weight. At the CPAP, plastic surgeons work in close coordination with paediatric anaesthetists, paediatricians, specialised nurses, and nutritionists. A burn ill managed, an ill-suited anaesthesia, a preventable infection may compromise months of effort. Yet the surgical act is but one stage. Rehabilitation is essential: physiotherapy, functional follow-up, at times orthotic support. Without it, scars contract anew, joints stiffen, progress is effaced. Psychological accompaniment is no less decisive. Among the youngest, it often concerns the parents. Guilt is frequent; stress likewise. In fragile family contexts, the accident may exacerbate tensions already present. To care for the child is also to sustain his environment. This comprehensive approach lies at the heart of the CPAP model: a paediatrics that heals without isolating, that reconstructs without dissociating.
Vulnerability as a Concrete Constraint
In Bolivia, many of the children cared for at the CPAP come from rural or peri-urban regions. Distance, the cost of transport, the necessity of remaining several weeks in the city constitute major obstacles. Families are often numerous. The hospitalisation of one child signifies the absence of a parent, at times of the mother, leaving the other children without support. The choice then becomes impossible: to remain in order to tend to one, or to depart in order to protect the others. Even when care is offered at social rates, the indirect costs—medicaments, lodging, loss of income—weigh heavily. During surgical campaigns, this reality is rendered into a difficult observation: not all the children assessed can be operated upon—not for want of medical indication, but for want of means. This constraint is not a medical failure. It is the reflection of a still fragmented health system, wherein access to specialised care remains unequal.
Technology, Prevention, and Pragmatism
In the face of these limits, each innovation bears weight. Modern dressings, for example, make it possible to space out treatment, to reduce the risk of infection and hospital costs. To pass from daily management to an intervention every five or seven days profoundly alters the organisation of care. Prevention remains another major concern. Holiday periods, when children spend more time at home, account for a large share of accidents. To raise awareness, to adapt domestic spaces, to secure kitchens—these are simple measures, yet still too little disseminated. Prevention pertains not to the medical sphere alone. It engages society, families, institutions. It presupposes an understanding of the realities of daily life rather than a judgement upon them.
When to Reconstruct Is to Restore the Future
The results of reconstructive surgery are not measured solely in centimetres of skin or in degrees of mobility restored. They are read in daily life. A child who can once more bend his arm, write, run. Another who returns to school without hiding himself. A family that regains its equilibrium after months of strain. At times, these results are contained within a simple image: that of a child filmed by his mother, walking once more through a neighbourhood market after long weeks of hospitalisation. An ordinary scene. A silent victory. For the medical teams, it is there that meaning appears—not in heroism, but in continuity. To do what must be done. With rigour. With humanity.
Trained in Bolivia and thereafter abroad, the surgeon who granted us this interview has chosen to devote an essential part of his practice to paediatric reconstruction. A deliberate choice. “Reconstructive surgery,” he says, “restores more than it takes. It is measured not in revenue, but in life trajectories regained.”
| The Albina R. de Patiño Centre of Paediatrics is inscribed within a long history—that of a steadfast commitment to paediatric health in Bolivia. Yet it acts resolutely in the present, with the tools of today and the challenges of tomorrow. Reconstructive surgery of burn sequelae is not a punctual response. It forms part of a broader vision: to offer children the conditions of a full development, despite the accidents of life. Here, it is not a matter of repairing the past. It is a matter of rendering the future |
“When a child can once more walk, play, return to school, we have done what we were bound to do.”